Generational Differences Among African Americans, Their Experiences with the Healthcare System
A study exploring healthcare preference and experience in this population group uncovers new insights and opportunities related to clinical research participation.
Image credit: DC Studio | stock.adobe.com

A large-scope research project outlined ahead identified and compared generational differences among African American adults and their experiences with the healthcare system. The study, conducted by CSL and CliniSpan Health, received 500 responses from African American adults and compared medical visit experiences, perceptions of safety and equitable treatment of patients within healthcare settings, clinical trial participation, and preferred methods of communication.
Results showed that most respondents seek out African American physicians and prefer medical offices with personnel who are African American. While most survey respondents believe the healthcare system is becoming safer, several respondents from Generation X spoke of past and current mistreatment of African American patients due to racial inequities. Most respondents believe that African Americans have been and continue to be treated differently than individuals of other races/ethnicities.
The reason most respondents gave for not participating in clinical trials was not a lack of trust or past mistreatment of study participants (i.e., the Tuskegee Syphilis Study) but rather the lack of knowledge surrounding clinical trial opportunities. And most respondents cited social media as their “go-to” place to find information about clinical trial opportunities, with Generation X citing Facebook groups and forums and Generation Z and Millennials listing TikTok and Instagram.
Identifying these preferred methods of engagement, as well as perceived barriers to healthcare and clinical research involvement is a crucial step to making clinical trials and healthcare more accessible for African American communities. This report discusses the process through which the survey was administered and the results.
Background
Increasing the number of African American physicians in primary and specialty care, as well as the number of African American clinical research staff at sites can increase African American patient willingness to engage in preventive healthcare procedures, receive treatment, and participate in clinical trials.1,2 Several historically black colleges and universities (HBCUs) have pledged to build medical schools in the last three years, and predominantly white institutions have been focusing on increasing the diversity of their medical student base.3
While these efforts are promising, relative to the 13% of the US population who are African American, the proportion of physicians who are African American has remained at 5% since the 1940s,4 and African Americans are the most under-represented demographic group in clinical trials at 5%. Three times as many African American participants should be enrolled in pivotal trials each year to achieve accurate representation related to disease prevalence and population census figures.5
Research has shown that the COVID-19 pandemic has created even greater gaps in disparities of care and health outcomes among African Americans and other racial and ethnic populations. The literature recognizes lesser access to quality medical care due to systemic racism and discrimination as a major reason for poorer health outcomes for African Americans.6
Younger African American women are more likely to say they have had negative healthcare experiences with non-African American physicians. In these encounters, they had to advocate for themselves to get proper care, were treated with less respect, and their level of pain was not taken seriously.
However, when African Americans have been asked in the past five years about whether they prefer African American physicians for routine and preventive care, the results have been mixed by gender and levels of education. Recent studies have shown that African American adults do not have a preference when it comes to the race and ethnicity of their care provider if they’re receiving high-quality care; however, younger African American women (18-49 years old) prefer African American physicians for routine care, and a similar preference was noted among individuals with higher levels of education (postgraduate and college degrees). Regardless of preference, African American patients are more likely to rate African American physicians with higher satisfaction levels than physicians of other racial and ethnic backgrounds.7
CSL and CliniSpan Health launched a new study to validate earlier healthcare preference and experience findings among African American adults, as well as identify generational differences related to clinical research participation. The FDA’s Diverse and Equitable Participation in Clinical Trials (DEPICT) Act, which requires pharmaceutical companies to include race and ethnicity diversity plans as part of regulatory submission packages,8 increases the need to understand preferred methods of communication, supportive services, and healthcare provider preferences to improve access to quality healthcare and clinical research among under-represented communities. This team plans to further explore preferences and needs of other demographic groups in future iterations of this research project.
Methods
Survey design and analysis planning were conducted and reviewed by CliniSpan Health and CSL between September 2022 and October 2022. Following review and approval by institutional review board Advarra, the survey was distributed to a US-based audience between October and December 2022. Survey distribution was conducted through email blasts to CliniSpan Health’s database of 2,500 people.
Thirty individual interviews were conducted between January and February 2023. Interviewees were selected from survey respondents to represent diversity in age, gender, socioeconomic, geographical, and educational backgrounds. Age groups were defined within the survey instrument and are provided in Table 1 as seen by respondents.
TABLE 1: Age Range by Generation
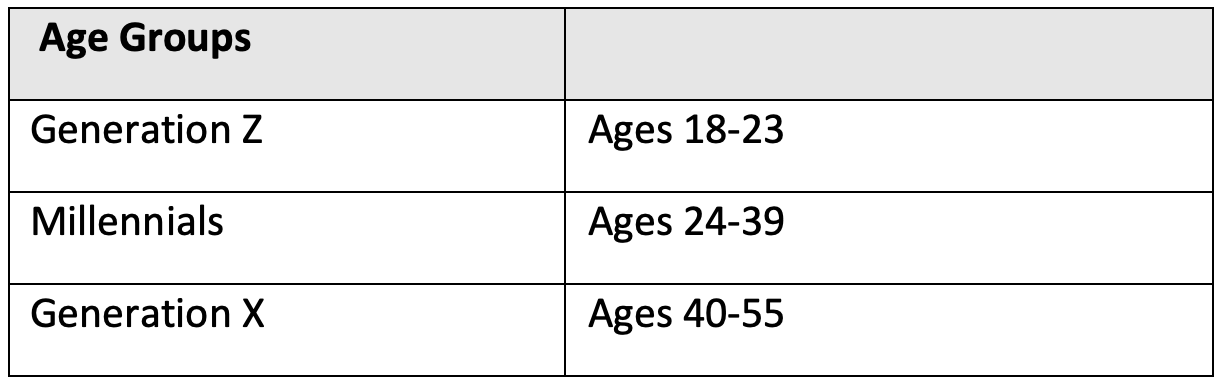
Raw data was stored and analyzed in Microsoft Excel. Analyses performed included frequency comparisons, comparisons of mean overall and subgroup response values, and correlations. Subgroups were created based on gender, highest degree earned by respondent, location, and household income.
Results
In total, 500 African American adult respondents consented to participate in the online survey. More than half (60%) of respondents completed a bachelor’s degree and a fifth (20%) completed an associate degree. Almost half (45%) of survey respondents earned $50,000 or more in annual household income; respondents were evenly split among gender demographics. Respondents were residents of New York, North Carolina, California, Texas, Minnesota, and Florida. Respondent characteristics are summarized in Table 2.
TABLE 2:Respondent Characteristics
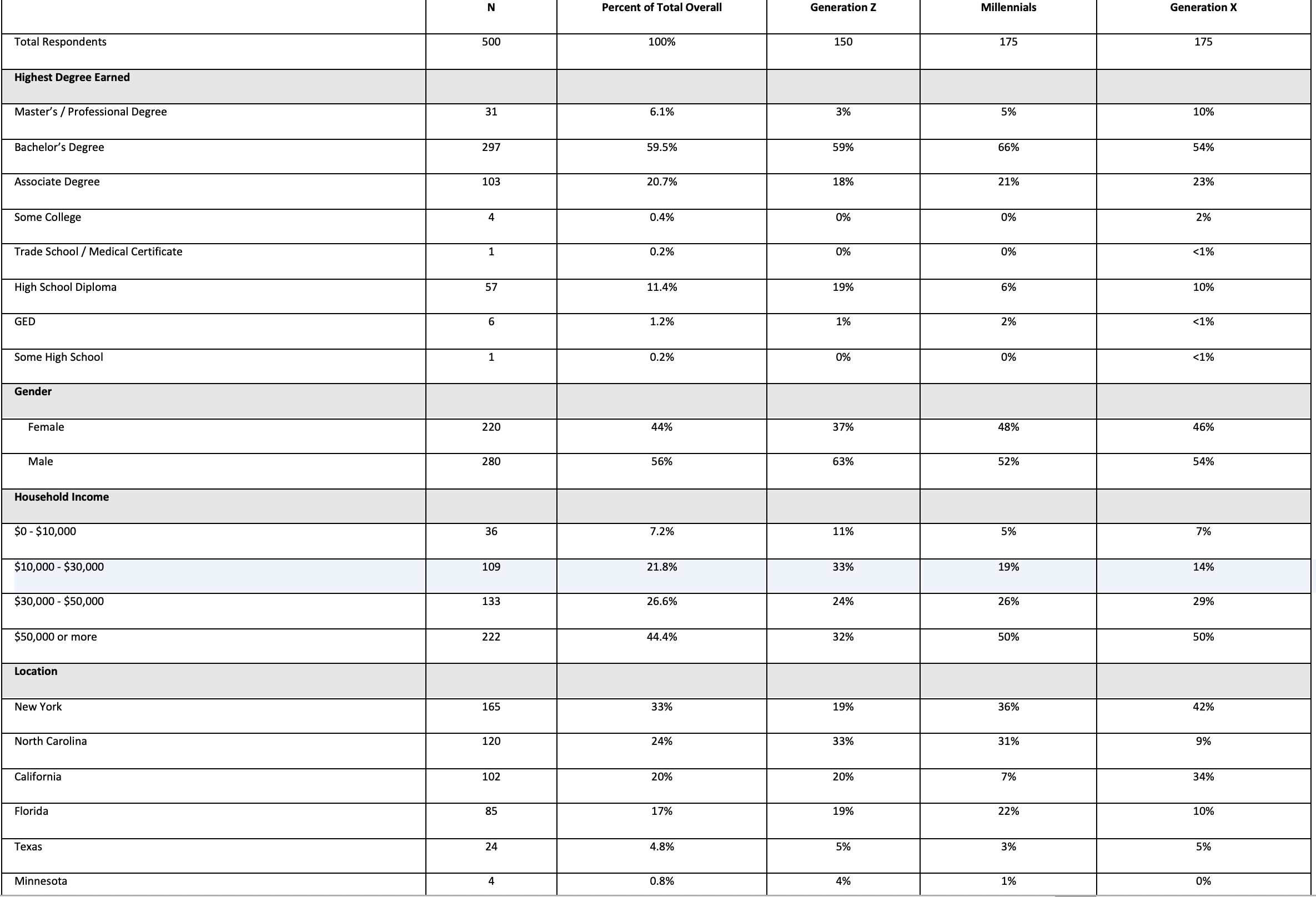
Health Care Experience and Preferences
Over half (59%) of survey respondents visit a doctor at least twice a year; most of these respondents (31%) represented Generation X (40-55 years old). Half of these respondents (53%) reported that they visit a family doctor due to ailments and long-term diseases, such as arthritis, asthma, and diabetes. Table 3 shows a breakdown of visit frequencies from all participants across Generations X, Millennials, and Z.
Table 3. Doctor Visit Frequencies Across Generations
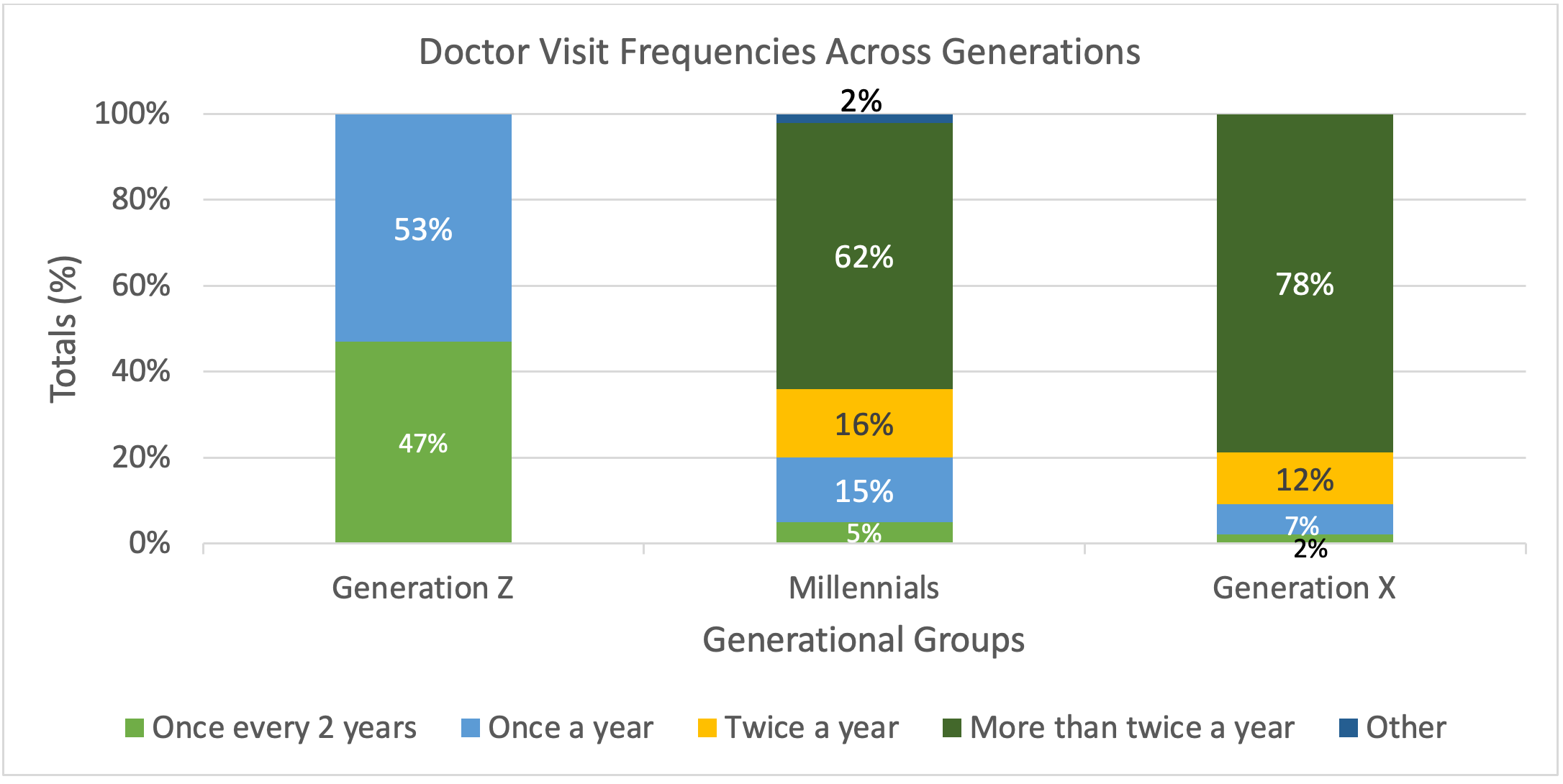
Half (53.8%) of respondents fully trust the healthcare field; over 40% of respondents who shared the greatest trust in the healthcare field were Millennials (24-39 years old). Generation X (40-55 years old) represented the small percentage (3%) of participants who do not trust the healthcare field (Table 4).
Table 4. Trust in the Healthcare System
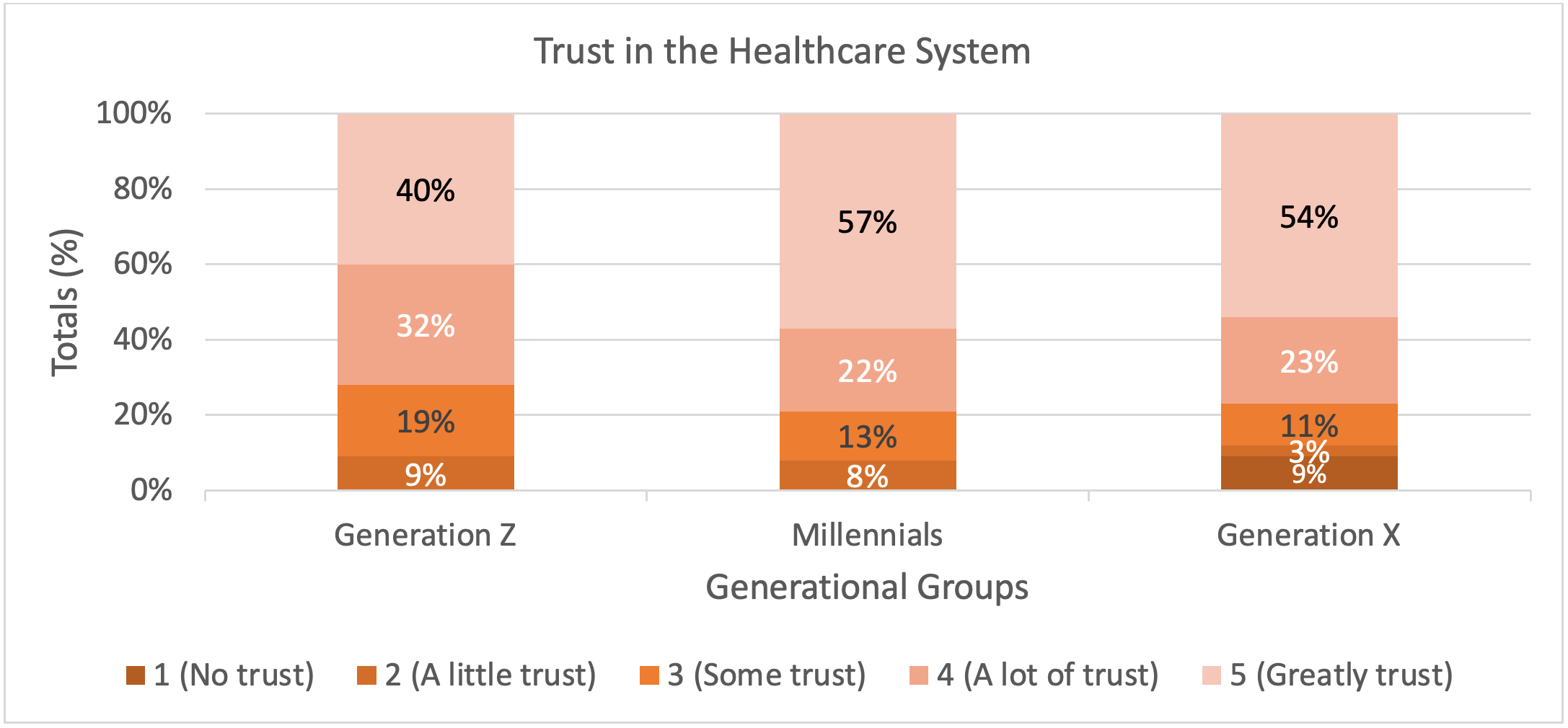
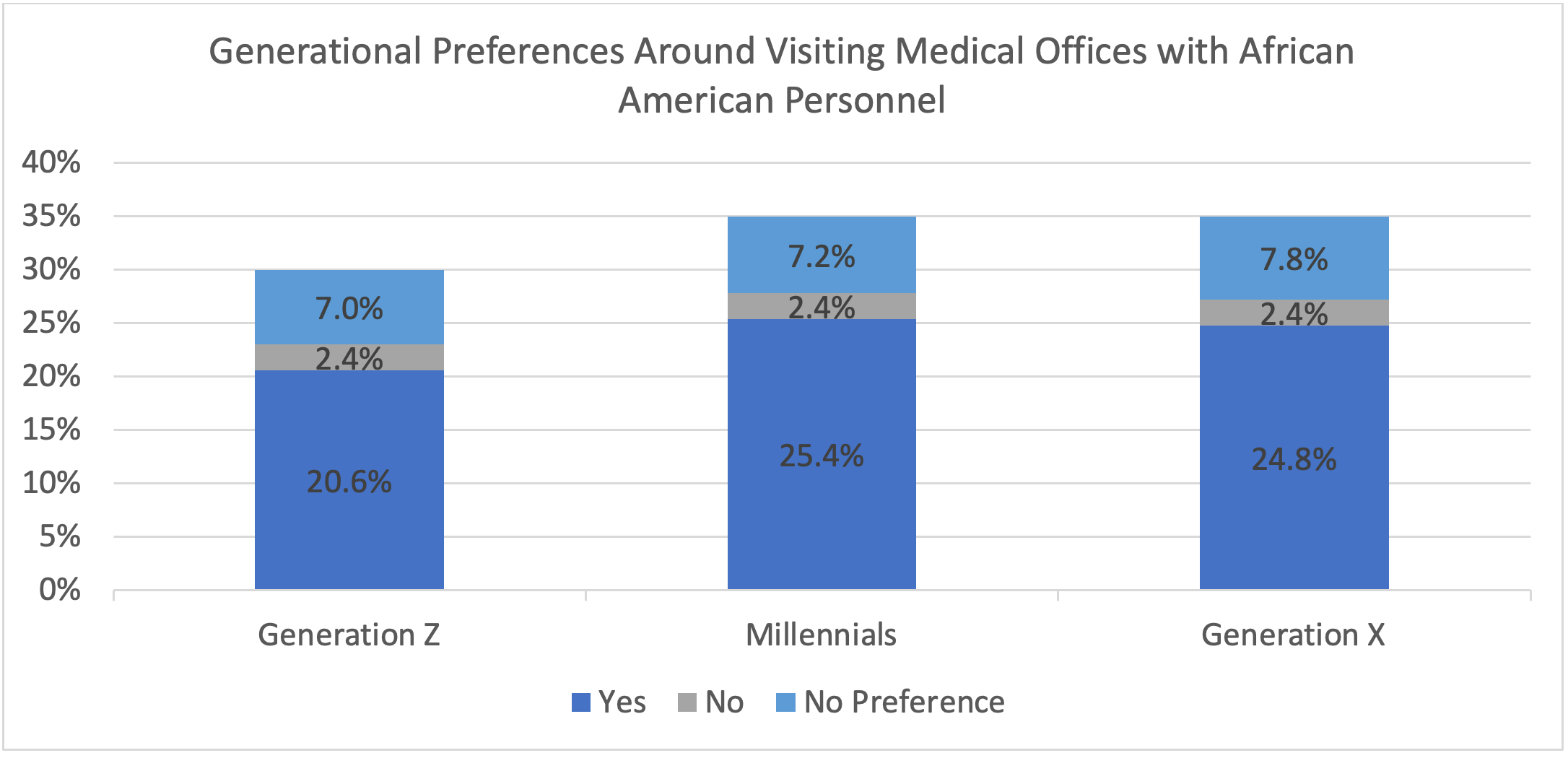
Almost 80% of respondents visit a primary care physician that is African American. Nearly 70% of respondents stated that they feel more comfortable or would feel more comfortable having an African American physician as their primary care physician. Most respondents (71%) prefer to visit medical offices with personnel who are African-American. See Table 5 for preferences across generations.
Table 5. Generational Preferences Around Visiting Medical Offices with African American Personnel
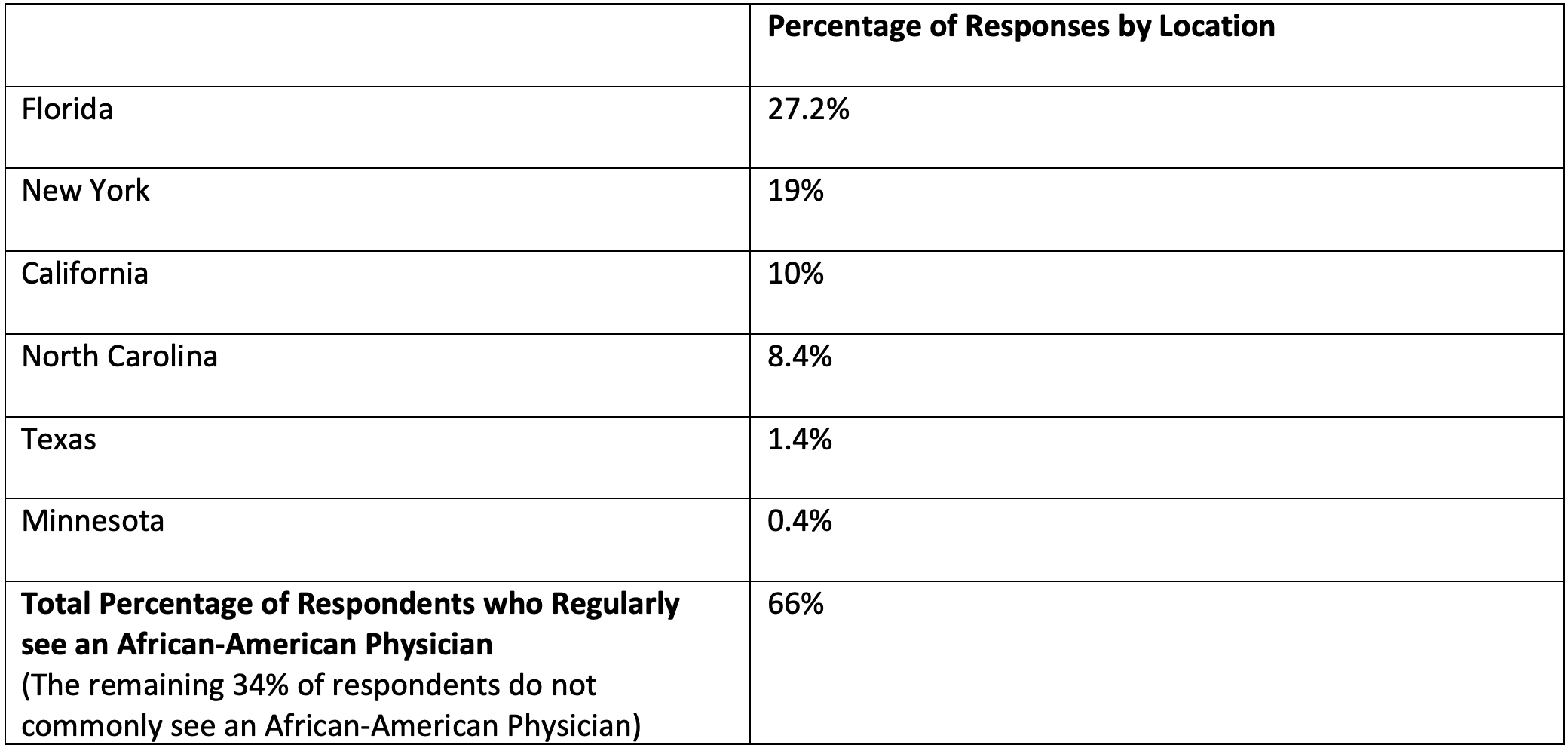
Respondents from Florida, New York, and California were most likely to report seeing an African American physician on a regular basis (Table 6).
TABLE 6: Top US States Where Respondents Report Seeing an African-American Physician on a Regular Basis
Almost all respondents (90%) trust African American physicians and reported excellent experiences with them. In consecutive interviews, respondents shared that African American physicians “give treatment willingly without discrimination” and they “tend to be more interactive and welcoming; they give off the feeling they want me there.”
Only 1% of Generation X (40-55 years old) respondents stated they had a terrible experience with an African American physician—and the poor rating did not relate to care received, but rather due to their experience in the medical clinic (i.e., longer wait times and a smaller facility).
Table 7 shows generational differences of perception about the quality of education received by African American physicians compared to Caucasian physicians.
Table 7. Perceived Education Levels of African American Medical Professionals Compared to Caucasian Medical Professionals
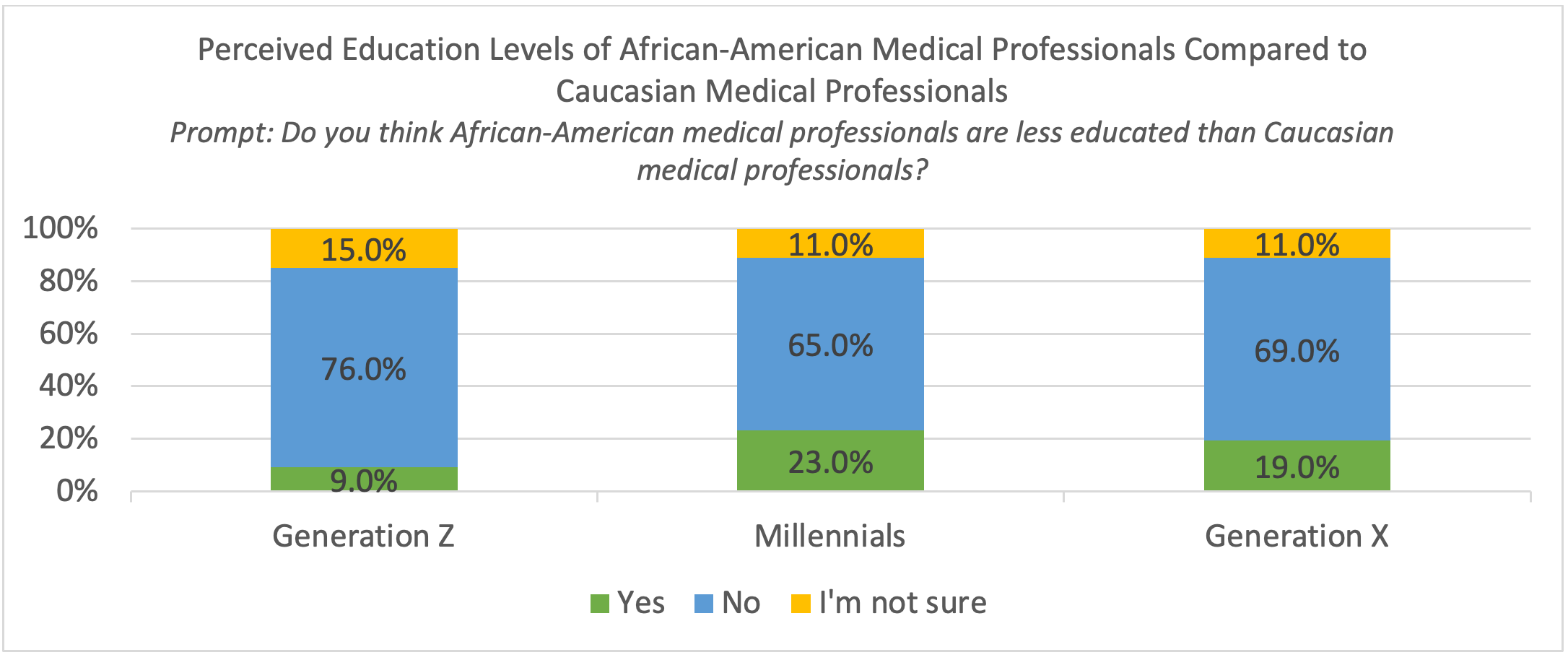
Most respondents (70%) do not think that African American medical professionals are less educated. Some Millennials and Generation Z respondents believe that African American medical professionals are more educated than peers of other races and ethnicities. There are some geographic locations where the view of medical professional education among African Americans is considered subpar. This is an area for additional research.
Historical Mistreatment of African-American Patients
Most Generation X (40-55 years old) respondents believe that African-American patients have been historically treated differently in medical facilities. Table 8 shows perceptions across the three generations. Respondents cited racial discrimination and lack of resources as main reasons for the mistreatment among African-American patients.
Table 8. Perceptions Around the Historical Mistreatment of African American Patients
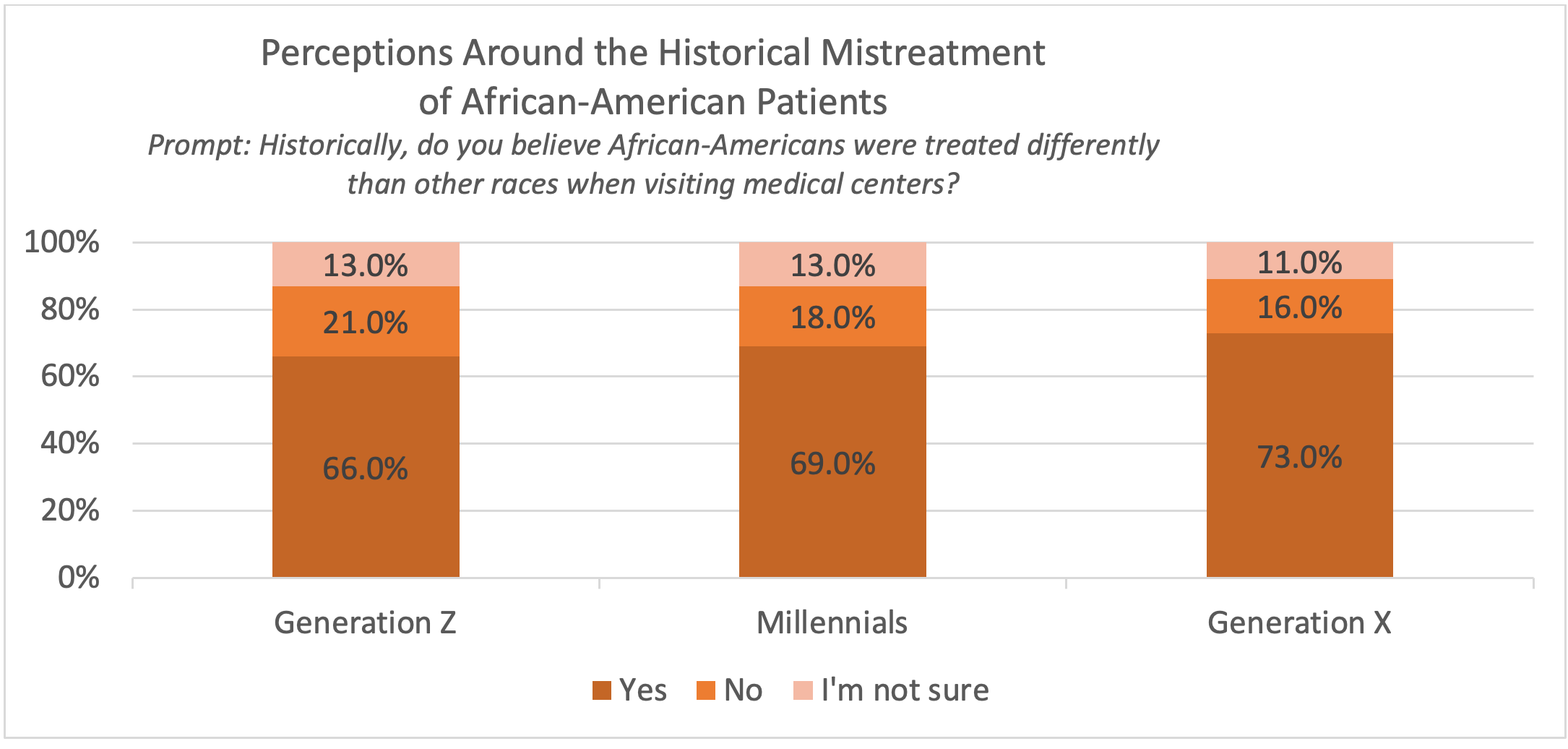
Other reasons shared were the lack of medical services available in predominantly African American neighborhoods; the US Public Health Service (PHS) and the Centers for Disease Control and Prevention (CDC)’s Tuskegee Syphilis Study; fewer numbers of African American doctors; societal racism toward African Americans; lack of access to medical treatment and medicine; and medical malpractice.
Half (50%) of respondents believe that African American patients are still treated differently in medical facilities. Younger generations believe that African American patients are treated more fairly than in the past. Nearly all respondents believe the healthcare system is becoming safer for African Americans.
Clinical trial participation
Most respondents (70%) have never participated in a clinical trial. The main reason for not participating is the lack of knowledge surrounding clinical trials. Most respondents did not know where to go to participate in a clinical study or what participating in a trial entails. A small number of respondents said lack of trust kept them from participating—a lack of trust that medical information would be kept confidential and a lack of trust in the clinical research enterprise.

When considering a clinical trial, social media was the most heavily cited source for information (81.6% of respondents). Generation X (40-55 years old) respondents selected Facebook as their No. 1 source, and many noted that they see clinical trials marketed on their news feeds. These respondents also noted that they seek disease-specific Facebook groups and forums to speak with others that are interested in participating in clinical research.
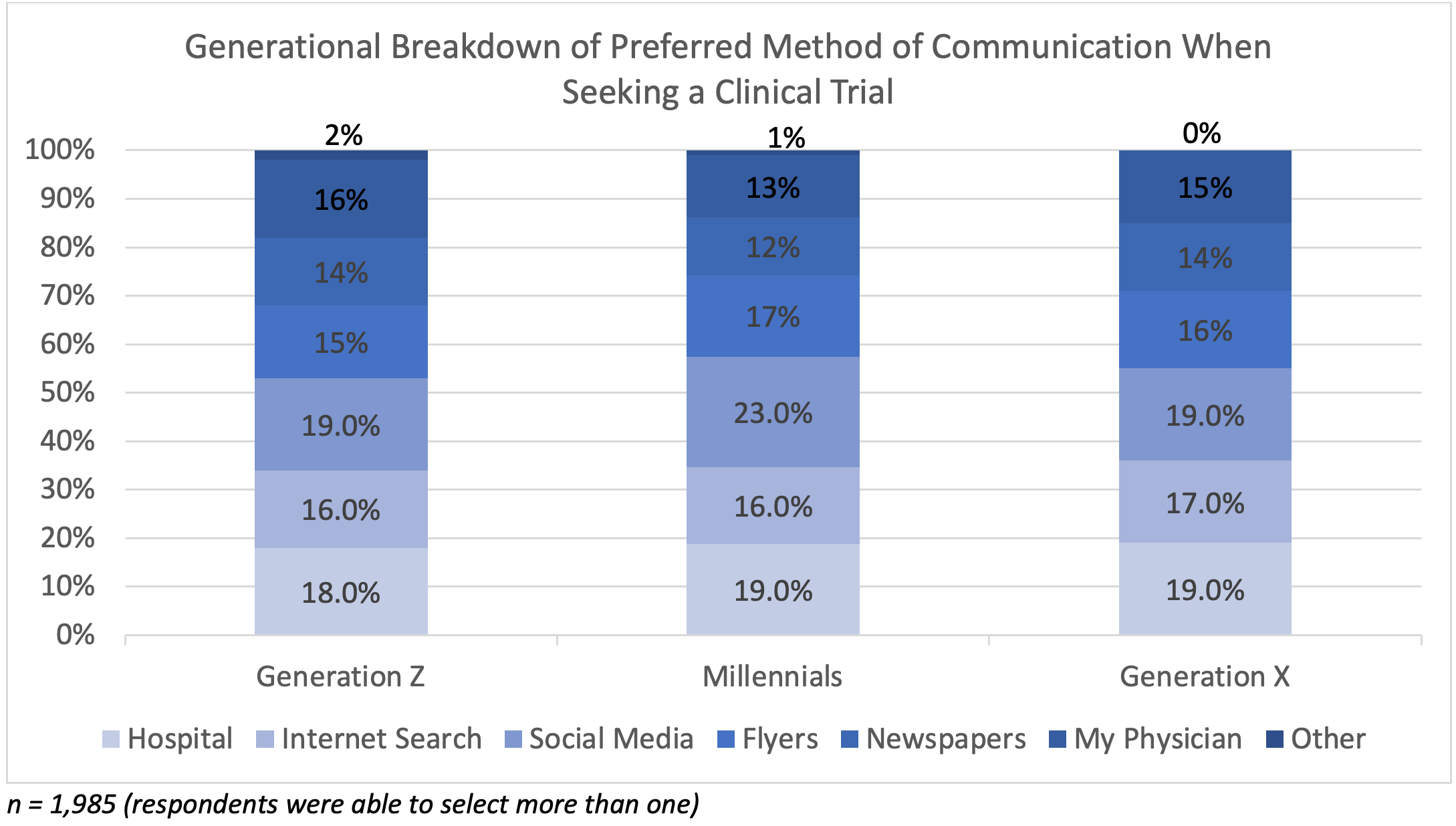
Generation Z (18-23 years old) and Millennials (24-39 years old) selected Instagram and TikTok as their most used social media platforms. Internet searches and flyers were less cited sources of information. Respondents in California and New York most often cited their physician as their primary source for information about clinical research. Table 9 shows preferred methods of communication for clinical trial opportunities among each generation.
Table 9. Generational Breakdown of Preferred Method of Communication When Seeking a Clinical Trial
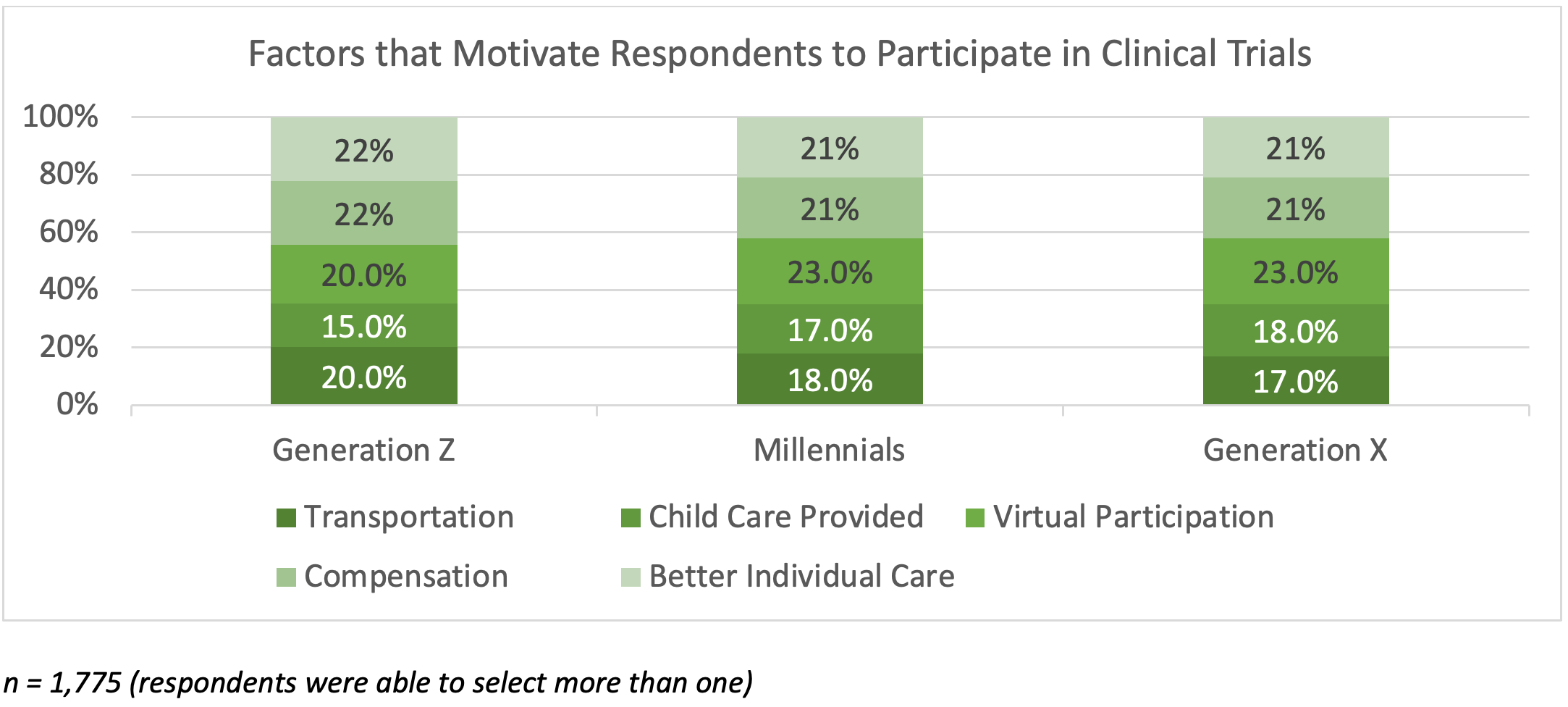
There is no single factor that respondents noted as a main incentive to participate in clinical trials. Regardless of generation, all respondents are looking for a collection of convenience and access opportunities, such as support through transportation, childcare, virtual participation, compensation for involvement in the study, and better individual care.
This is supported by other studies that have shown that there is no simple, standardized solution to encourage people to learn about and participate in clinical trials: people want a comprehensive, positive experience with flexible options that enable their participation to fit into their regular routine (Table 10).
Table 10. Factors that Motivate Respondents to Participate in Clinical Trials

Discussion
Over the last five years, publications have exposed the lack of racial and ethnic diversity among principal investigators in the US and medical professionals providing routine and preventive care. The literature also speaks to systemic racism and discrimination that hinder African American patients’ access to healthcare, clinical trials, and physicians who express interest in conducting trials. Our study offers insights into increasing equity in healthcare access and clinical research participation among African Americans.
First, this study shows that while African Americans across all generations believe healthcare is becoming a safer environment, they still regularly report acts of mistreatment. Healthcare institutions have an opportunity and an obligation to recognize biases among staff and transform organizations into models of equitable healthcare treatment and delivery.
The Harvard Kennedy School recently launched a framework for academic hospitals, public health agencies, and community health centers to implement policies, training tools, and supportive services to achieve sustainable change through antiracist practice.9 A link to this report and summary of findings is available in the reference section.
Second, a large gap exists between what researchers think they are sharing regarding clinical research opportunities and what African Americans want to receive to inform their decision to participate. While earlier industry assumptions have pointed to past abuses and mistreatment of African Americans as the main reason for a lack of participation,10 the lack of awareness around clinical research education and trials from trusted medical sources positively correlates to the lack of clinical research participation among African Americans from all age groups.
Our findings identify where healthcare professionals (HCPs), research teams, and pharmaceutical companies are falling short and reveal a major opportunity to make healthcare and clinical trials more accessible. African Americans participants in our research say they want to receive information about their health and clinical research opportunities from social media (Facebook for older generations and TikTok and Instagram for younger generations) and from their trusted care physician and family doctor.
While social media has its role to play, pharmaceutical companies need to further invest communications that support the doctor-patient relationship and the physician’s important role in sharing clinical research opportunities with them.11 Pharmaceutical companies should assist by co-developing digital and printed one-pagers that give physicians the information they need to quickly evaluate clinical research studies for their patients.
Clinical research sponsors also have a major opportunity to focus on disease prevalence among racially and ethnically diverse communities and site staff diversity within early planning stages and preliminary feasibility in order to ensure a more diverse representation among study participants. This will add to what US clinical trial sites are already doing to actively engage with and recruit ethnically and racially diverse community members through local events, engage community health centers to serve as satellite research facilities, and employ mobile research sites.
Third, our study recognized that African Americans across all age groups and genders say they want to receive care from African American medical professionals, despite recent publications suggesting a lack of preference. In individual interviews, survey respondents offered numerous accounts that spoke to the importance of a shared history and culture.
Many interviewees shared that medical professionals with shared cultural values and traditions are more likely to understand their behaviors and customs, and they are more successful in communicating and encouraging relevant treatment options. Therefore, it’s even more essential for HBCUs to build medical schools; for historically white institutions to increase racial and ethnic diversity; and for all healthcare institutions—especially medical schools, hospitals, academic medical centers, and research sites—to offer more mentorship and training opportunities that are culturally sensitive for diverse staff.
A recent Tufts Center for the Study of Drug Development study showed a positive correlation among clinical research staff diversity and the diversity of participants enrolled in studies.12 Our findings offer insights for pharmaceutical companies regarding site feasibility and identifying site stakeholders with diverse staff and community engagement activities. Our findings also can inform health institutions as they conduct staff training and increase access to jobs for diverse medical professionals.
Given these results, we remain optimistic about the momentum behind increasing diversity among medical professionals across the healthcare continuum, patients, and study participants. Future research would be informative if it identified the resources HCPs need to alert patients about clinical trials and conducted a study among African American respondents who are not as tech-savvy in navigating their health care.
Additionally, we are interested in further understanding the types of information that prospective participants want to receive about clinical trials and health care across many channels, including social media, mass media, direct conversations with doctors, and flyers at gyms, libraries, and community facilities. We also would like to better understand which support services would be most beneficial to stand up across therapeutic indications so that pharmaceutical companies can build relevant, meaningful trials around participant routines and lives.
Conclusions
Increasing the number of African American physicians in primary and specialty care, as well as the number making up research staff at sites, can increase African American patient willingness to engage in preventive healthcare procedures, receive treatment, and participate in clinical trials. Age and gender did not offer significant differences in perception of healthcare and clinical research participation.
African Americans of all age groups prefer doctors who will offer high quality care, will take their symptoms and pain seriously, and will advocate for their health. Social media was a major healthcare education and clinical trial recruitment channel utilized by individuals across all age groups—with Facebook as a main platform for Generation X and Tik Tok and Instagram main platforms for Generations Z and Millennials. Future phases of this research initiative will encourage more diverse participation (via printed and call-in surveys among other demographic groups) and a separate study related to the key educational components needed by HCPs to more confidently evaluate clinical research options for their patients.
About the Authors
Ellyn Getz, MPH, is Director, R&D Patient Partnerships, R&D Strategic Operations, CSL; Rodney Winley, MBA, is Senior Director, R&D Patient Partnerships, CSL; VeQuain Joyner is Director of Business Development, CliniSpan Health; and Dezbee McDaniel is Cofounder and CEO, CliniSpan Health
Study limitations
This study was not without limitations. The biggest limitation stemmed from the primary recruitment channel for survey participation, which was through the CliniSpan Health platform. This opt-in platform regularly engages African American community members about clinical research opportunities and recruits through social media platforms, influencers, and word of mouth.
While the database hosts over 2,500 users, this recruitment channel was limited to the main geographical areas within which CliniSpan has created hubs, as well as mainly targeted survey respondents who were digitally savvy and health conscious.
The survey also recognized varying levels of knowledge among respondents surrounding clinical trial participation. An assumption while creating the survey instrument was that each respondent had a basic knowledge of what clinical research entails based off their opt-in to learn about clinical trial opportunities through CliniSpan Health. Structured interviews, however, recognized a need for further education regarding the clinical research process.
Future studies may wish to utilize different recruitment channels to engage with a more diverse cohort of respondents, such as flyers at local community centers, libraries, restaurants, beauty salons, and barber shops with a number for a phone-based survey and representation at community events to pass out paper surveys. These grassroots settings—especially hair salons and barber shops—enable open dialogue between trusted community members and have proven to be successful in promoting health and wellness.13,14 For online and in-person surveys, brief information around the clinical research process with visual aids and audio may help align respondent understanding and expectations.
Funding
This study was funded by a grant provided by CSL.
Acknowledgements
The authors would like to thank Deirdre BeVard; Jamilah Dawkins; Michael Galloway; Ken Getz, MBA; Dominick Harris; David Lipsitz, MD; Debra Moffitt; and Madison Reider for their contributions and invaluable input to this research project.
References
1. Nadeem, R. (2023) Black Americans' Views About Health Disparities, Experiences with Health Care. Pew Research Center Science & Society. Pew Research Center. Available at: https://www.pewresearch.org/science/2022/04/07/black-americans-views-about-health-disparities-experiences-with-health-care/ (Accessed: May 27, 2023).
2. Botto; E.; Kim, J.; Foster, Z.; et al. (2022) Improving Diversity in Clinical Trial Volunteer Participation by Addressing Racial and Ethnic Representation Among the Clinical Research Workforce. Applied Clinical Trials. Available at: https://www.appliedclinicaltrialsonline.com/view/improving-diversity-in-clinical-trial-volunteer-participation-by-addressing-racial-and-ethnic-representation-among-the-clinical-research-workforce (Accessed: January 21, 2023).
3. Steele, D. (2022) New Med Schools Planned as Need for Black Doctors Continues. Inside Higher Ed | Higher Education News, Events and Jobs. Available at: https://www.insidehighered.com/news/2022/05/13/new-med-schools-planned-need-black-doctors-continues (Accessed: 15 April 2023).
4. Ly, D. Historical Trends in the Representativeness and Incomes of Black Physicians, 1900-2018. J Gen Intern Med. 2021. doi:10.1007/s11606-021-06745-1
5. Getz, K.; Smith, Z.; Pena, Y. (2020) Quantifying Patient Subpopulation Disparities in New Drugs and Biologics Approved Between 2007 and 2017, Therapeutic innovation & Regulatory science. US National Library of Medicine. Available at: https://pubmed.ncbi.nlm.nih.gov/32557009/ (Accessed: April 7, 2023).
6. Williams, D.R.; Rucker, T.D. (2000) Understanding and Addressing Racial Disparities in Health Care. Health Care Financ Rev. US National Library of Medicine. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4194634/ (Accessed: April 7, 2023).
7. Takeshita, J.; Wang, S.; Loren, A.W.; et al. Association of Racial/Ethnic and Gender Concordance Between Patients and Physicians with Patient Experience Ratings. JAMA Netw Open. 2020. 3 (11), e2024583. doi:10.1001/jamanetworkopen.2020.24583
8. H.R.6584 - 117th Congress (2021-2022): DEPICT act (2022) H. R. 6584. Available at: https://www.congress.gov/bill/117th-congress/house-bill/6584 (Accessed: August 17, 2023).
9. Muhammad, K.G. (2023) Antiracist Institutional Change in Healthcare - ash.harvard.edu, Research Reveals Path to Effective Antiracist Change in American Healthcare. Available at: https://ash.harvard.edu/sites/hwpi.harvard.edu/files/ash/files/330395_hks_policy_brief_antiracism_web.pdf?m=1680201352 (Accessed: March 27, 2023).
10. Scharff, D.P.; Mathews, K.J.; Jackson, P.; et al.(2010) More than Tuskegee: Understanding Mistrust About Research Participation, J Health Care Poor Underserved. US National Library of Medicine. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4354806/ (Accessed: April 7, 2023).
11. Getz, K. (2017) Examining and Enabling the Role of Health Care Providers as Patient Engagement Facilitators in Clinical Trials. Clin Ther. US National Library of Medicine. Available at: https://pubmed.ncbi.nlm.nih.gov/29079388/ (Accessed: April 7, 2023).
12. Botto; E.; Kim, J.; Foster, Z.; et al. (2022) Improving Diversity in Clinical Trial Volunteer Participation by Addressing Racial and Ethnic Representation Among the Clinical Research Workforce. Applied Clinical Trials. Available at: https://www.appliedclinicaltrialsonline.com/view/improving-diversity-in-clinical-trial-volunteer-participation-by-addressing-racial-and-ethnic-representation-among-the-clinical-research-workforce (Accessed: January 21, 2023)
13. Releford, B.J.; Frencher, S.K; Yancey, A.K. (2010) Health Promotion in Barbershops: Balancing Outreach and Research in African American Communities. Ethn Dis. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4244298/ (Accessed: August 4, 2023).
14. Palmer, K.N.B.; Okechukwu, A.; Mantina, N.M.; et al.(2022) Hair Stylists as Lay Health Workers: Perspectives of Black Women on Salon-Based Health Promotion. Inquiry. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9016565/ (Accessed: August 4, 2023).
Newsletter
Stay current in clinical research with Applied Clinical Trials, providing expert insights, regulatory updates, and practical strategies for successful clinical trial design and execution.
Improving Relationships and Diversifying the Site Selection Process
April 17th 2025In this episode of the Applied Clinical Trials Podcast, Liz Beatty, co-founder and chief strategy officer, Inato, discusses a number of topics around site engagement including community-based sites, the role of technology in improving site/sponsor relationships, how increased operational costs are impacting the industry, and more.
Reaching Diverse Patient Populations With Personalized Treatment Methods
January 20th 2025Daejin Abidoye, head of solid tumors, oncology development, AbbVie, discusses a number of topics around diversity in clinical research including industry’s greatest challenges in reaching diverse patient populations, personalized treatment methods, recruitment strategies, and more.